Insulin Sensitivity: The Hidden Driver of Energy, Fat Loss, and Long-Term Health
Insulin sensitivity determines how efficiently your body responds to insulin — the hormone that controls blood sugar and energy balance.
When sensitivity is high, your body uses glucose efficiently, keeping energy stable and metabolism optimized.
When it declines, the body compensates by producing more insulin — leading to fat storage, energy crashes, and long-term metabolic stress.
Why Insulin Sensitivity Matters?
What Happens If Insulin Sensitivity Declines?
Chronic low insulin sensitivity (insulin resistance) develops gradually and often goes unnoticed for years. Over time, it disrupts multiple systems in the body and increases the risk of serious metabolic conditions.
This process often starts silently, without obvious warning signs.
Insulin resistance is present in up to 70% of individuals with obesity and is a major driver of metabolic syndrome (CDC, WHO).
How Insulin Sensitivity Works?
Insulin signals your cells to absorb glucose from the bloodstream. When sensitivity is high, this process works efficiently and keeps energy levels stable.
When sensitivity declines, cells respond less effectively. The body compensates by producing more insulin, leading to elevated blood sugar, increased fat storage, and long-term metabolic stress.
Over time, this creates a cycle of worsening insulin resistance and reduced metabolic efficiency.
Signs of Low Insulin Sensitivity →
Frequent Energy Crashes
Sudden drops in energy, especially after meals, often caused by unstable blood sugar levels.
Strong Sugar Cravings
Persistent cravings for sweets or refined carbs due to poor glucose regulation.
Difficulty Losing Fat
Stubborn weight, especially around the abdomen, despite diet or exercise efforts.
Brain Fog & Low Focus
Difficulty concentrating and mental fatigue linked to blood sugar instability.
Are You Likely Insulin Resistant?
If you recognize multiple signs, it may be worth assessing your insulin sensitivity through simple blood markers.
How to Improve Insulin Sensitivity Naturally?
Improving insulin sensitivity is not about extreme diets or short-term hacks. It is primarily driven by consistent lifestyle patterns that regulate blood sugar, reduce metabolic stress, and improve how your body responds to insulin over time.
The most effective strategies are simple, evidence-based, and sustainable.
RELATED TOPICS
Insulin sensitivity is influenced by multiple interconnected systems in the body.
Explore the key areas that shape metabolic health, from physical activity and nutrition to long-term weight regulation.
Metabolic Flexibility
Switch between fat and glucose efficiently — a core marker of metabolic health.
Weight Regulation
Insulin sensitivity directly impacts fat storage, hunger, and long-term weight control.
Metabolic Guide
Training strategies that improve insulin response and metabolic performance.
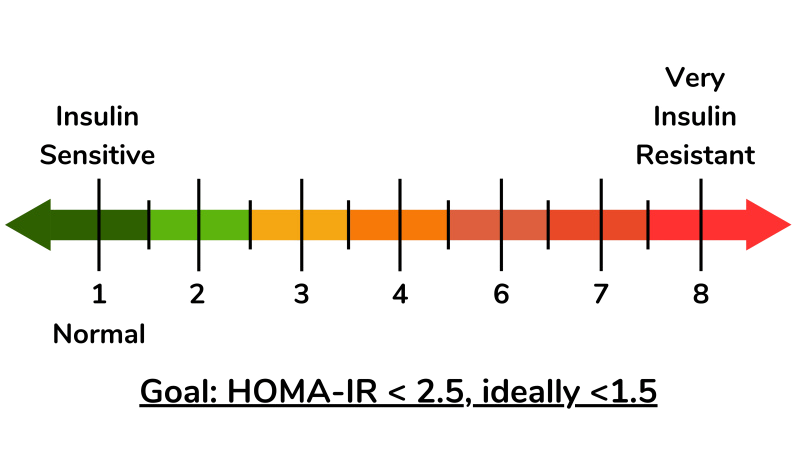
How to Measure Insulin Sensitivity
The most reliable indicators include fasting insulin, blood glucose, and calculated indexes such as HOMA-IR.
What Research Shows
01/
Regular exercise can increase insulin sensitivity by up to 40% (Journal of Applied Physiology)
02/
Resistance training improves glucose uptake even without weight loss (Harvard Medical School)
03/
Lifestyle interventions can reduce diabetes risk by up to 58% (Diabetes Prevention Program, NIH)
Two Paths of Metabolic Health
Metabolic Stress Path
Chronic overeating, poor sleep, stress, and lack of movement gradually reduce insulin sensitivity.
This leads to unstable energy, increased fat storage, and higher long-term disease risk.
Metabolic Efficiency Path
Consistent movement, balanced nutrition, and recovery improve how your body uses insulin, supporting stable energy and long-term metabolic health.






